Breast augmentation surgery, also known as augmentation mammoplasty, is a cosmetic surgery procedure that involves the placement of breast implants to increase the size and shape of the breasts. Breast Enhancement, breast augmentation or breast enlargement is also known as a ‘Boob Job’.
Specialist Plastic Surgeon Dr Mark Doyle offers a large variety of breast implant types and options to suit your anatomy. He is an experienced specialist plastic surgeon located in the Gold Coast, Queensland, with over 30 years of experience. Within the Gold Coast Plastic Surgery clinic, you will find a team of highly experienced Registered Nurses, our Registered Nurses work alongside Dr Doyle, to ensure you receive exceptional care both pre and post-surgery, in a supportive environment. With over three decades of experience, we are here to help you achieve your surgery goals.

What Is Breast Augmentation (Boob Job) Surgery?
Breast Augmenation, at a glance
Target area: Size and shape of the breasts
Time off work: 1-2 weeks
Total recovery: 6-weeks
Compression garment: 2 weeks full-time wear, 6 weeks total
Scar position: Along the fold beneath the breast
Breast augmentation (boob job) is a cosmetic procedure designed to increase the size and shape of your breasts. Although, there are several things to consider when deciding to undergo breast enlargement surgery. There are a large number of options when it comes to having a breast augmentation, or ‘boob job’, including breast implant choice and surgical techniques. Depending on your surgery expectations, Dr Doyle will discuss the options with you during your surgery consultation.
Consultation
During your initial surgery consultation at Gold Coast Plastic Surgery located on the Gold Coast, Queensland. With your surgery goals in mind, Dr Doyle will assist you in recommending a suitable breast implant size and shape. After measuring the dimensions of your breasts, he will have you try on several trial breast implants. So you can get an idea of what the final results will look and feel like.
Also, within your consultation, Dr Doyle will discuss your surgical options, the procedure, risks and recovery from breast augmentation. He will then answer any questions you may have about the breast augmentation surgery. Following your surgery consultation, you will receive all the information you need to make an informed decision about breast augmentation surgery (boob job).
If you are a smoker, you must stop smoking at least three months before surgery, and continue to abstain during your surgery recovery. Nicotine causes the blood vessels to shrink, compromises the function of red blood cells, and lowers oxygen levels in the blood. Cells must divide and grow for wounds to heal. Without adequate oxygen, this process can be delayed considerably.
Good Candidate
You may be a good candidate for a breast augmentation surgery if your breasts:
- Have mild breast ptosis
- Minimal breast tissue
- Low volume
- Uneven or asymmetry
- Reduced upper pole cleavage
- Sharp breasts with swollen nipples (tuberous breasts)
- Or if you would like to increase the size and shape of your breasts
It is very important to communicate with your surgeon before the surgery to ensure you have realistic expectations of the surgical outcome.
Want more assistance? Book your initial consultation or take our breast surgery quiz today to determine if you’re a good candidate for a breast augmentation (boob job) on the Gold Coast.
What Are The Benefits of a Breast Augmentation (Boob Job)?
Breast augmentation is a surgery procedure that can increase the breast size, chest size, breast side profile, breast shape and the location of your nipples (in a procedure called nipple reshaping).
The main benefit of undergoing breast augmentation is changing the way that you look. An enlarged chest will change your body proportions and add balance to your figure. According to a long-term study by Clinical Psychological Science, patients displayed increased enjoyment of life and satisfaction after having their physical appearance surgically altered.
Is Breast Augmentation a Major Surgery?
Yes, breast augmentation is a major surgical procedure. It can increase the size and shape of a woman’s breast. There are a large number of options with breast augmentation, including breast implant options and surgical techniques. Dr Doyle will discuss these options with you, to ensure they are in line with your surgery expectations.
Breast augmentation surgery generally takes an hour. The location of the incisions depends on your anatomy, surgery goals, and the type of breast implant you choose. At Gold Coast Plastic Surgery, we make every effort to ensure that your incisions are as minimal as possible. During breast augmentation surgery, Dr Doyle will create a space also known as a pocket, under the breast. He will put the implant either behind or in front of the chest muscle, depending on the results that you prefer. Most patients receive dissolvable stitches and generally, Dr Doyle performs it as a day surgery procedure at John Flynn Private Hospital.
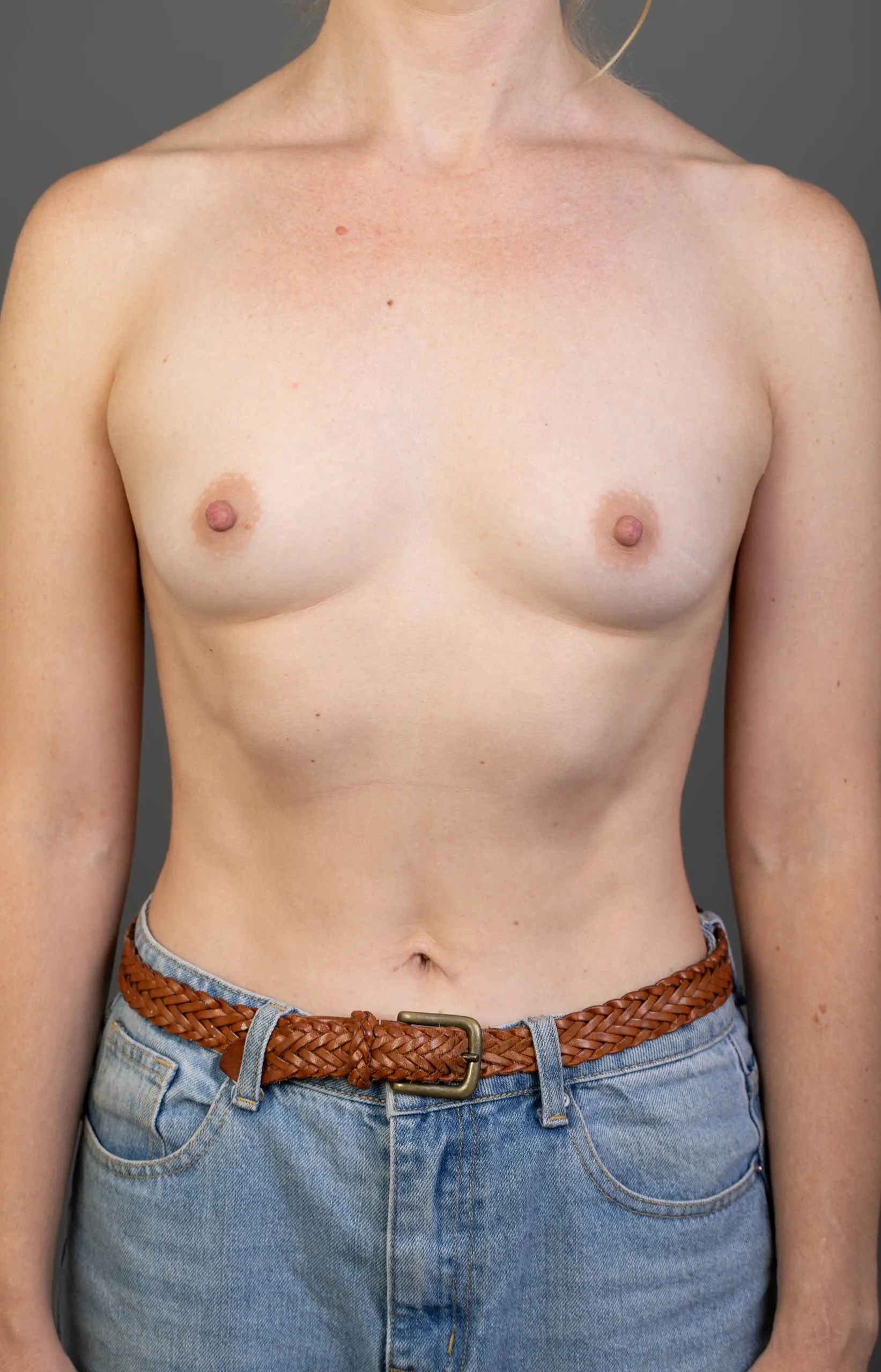
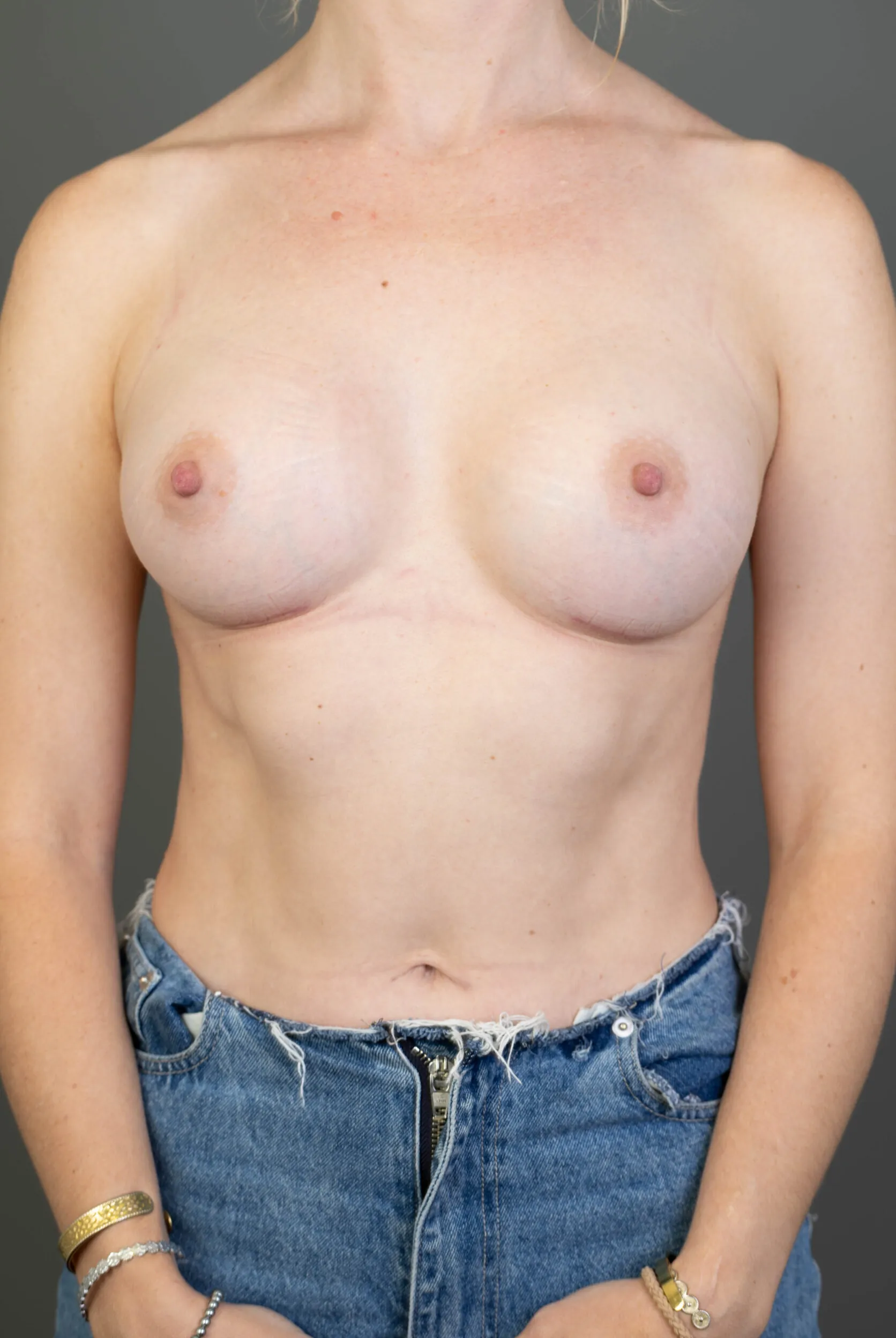
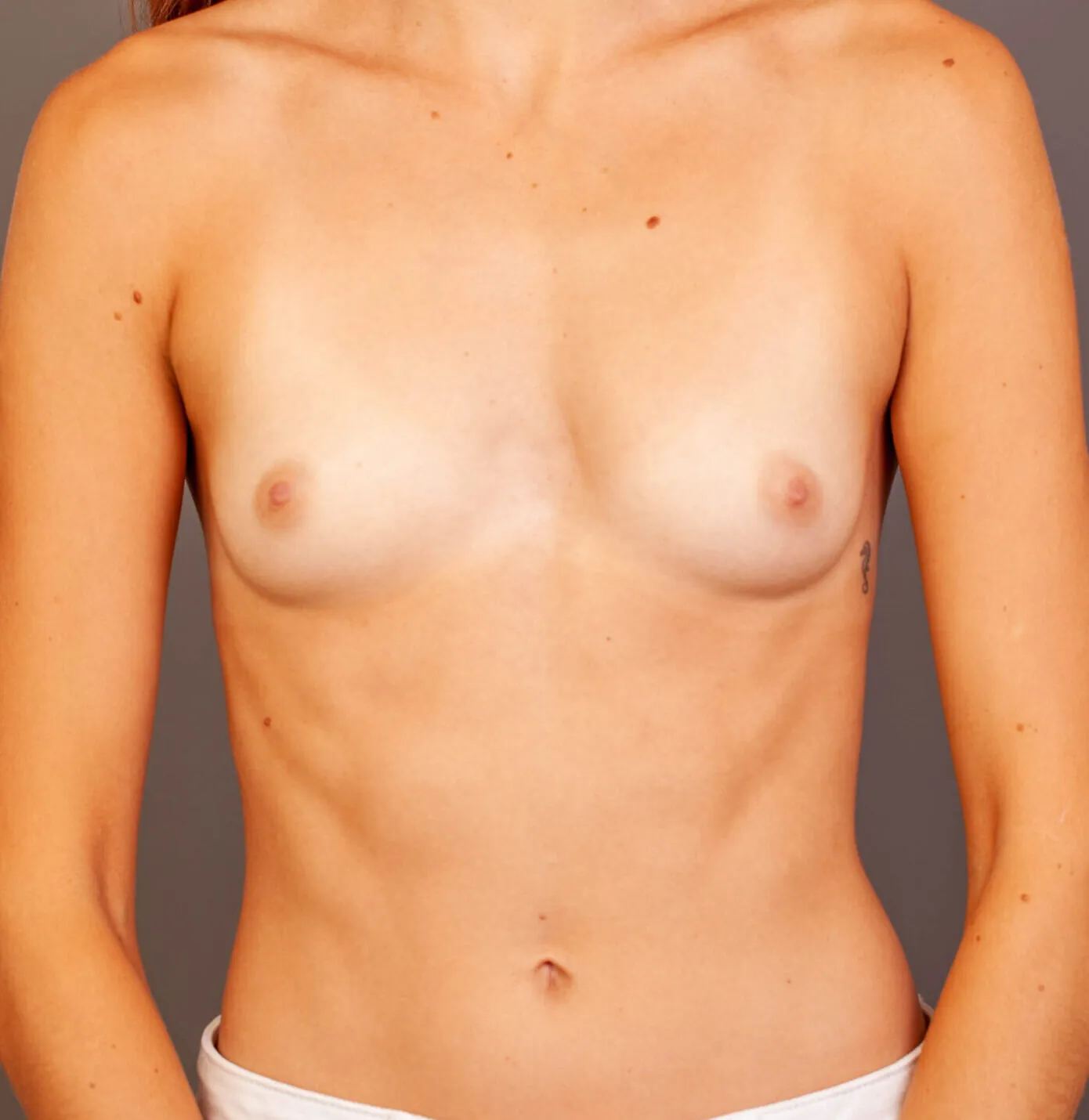
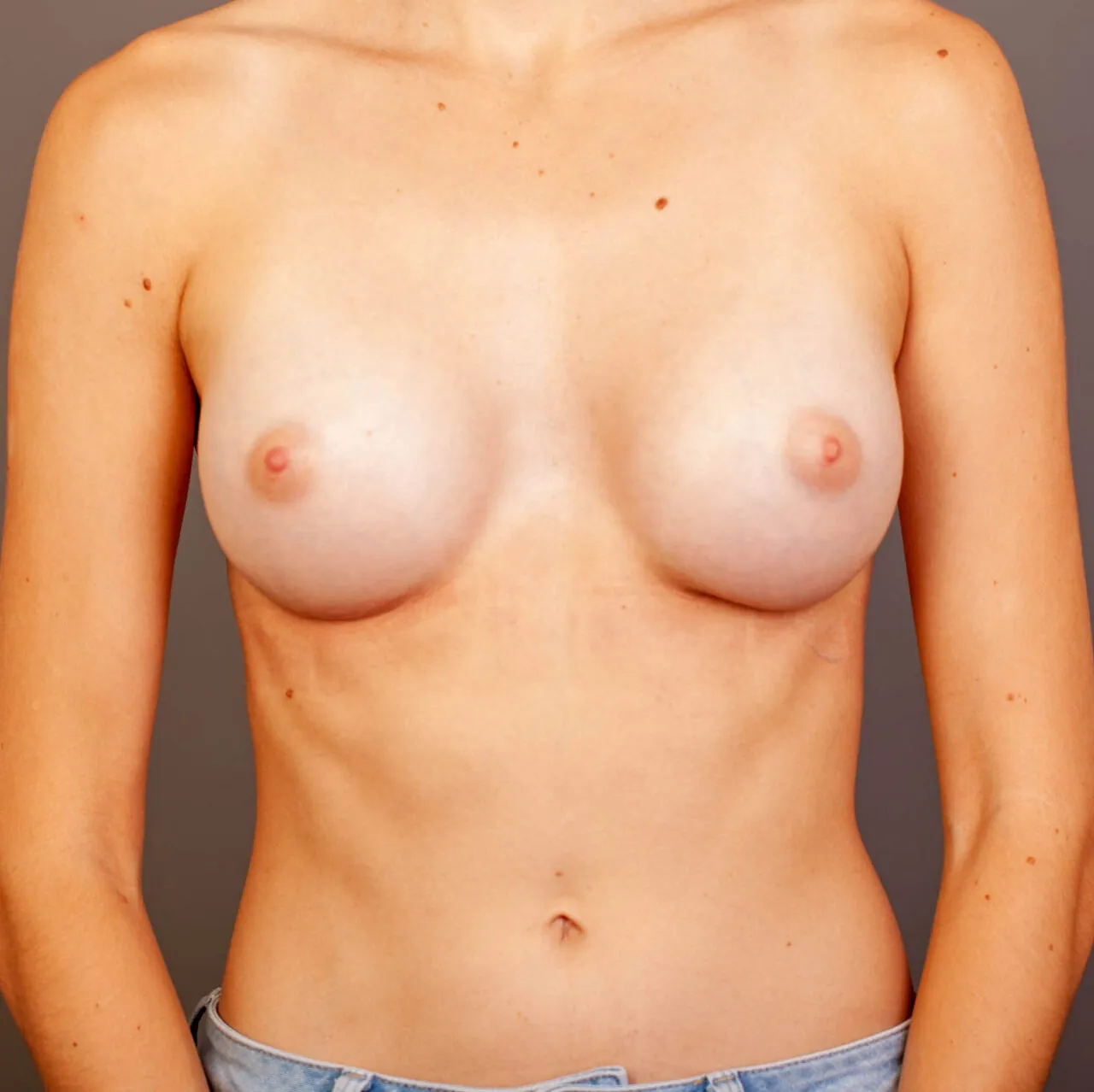
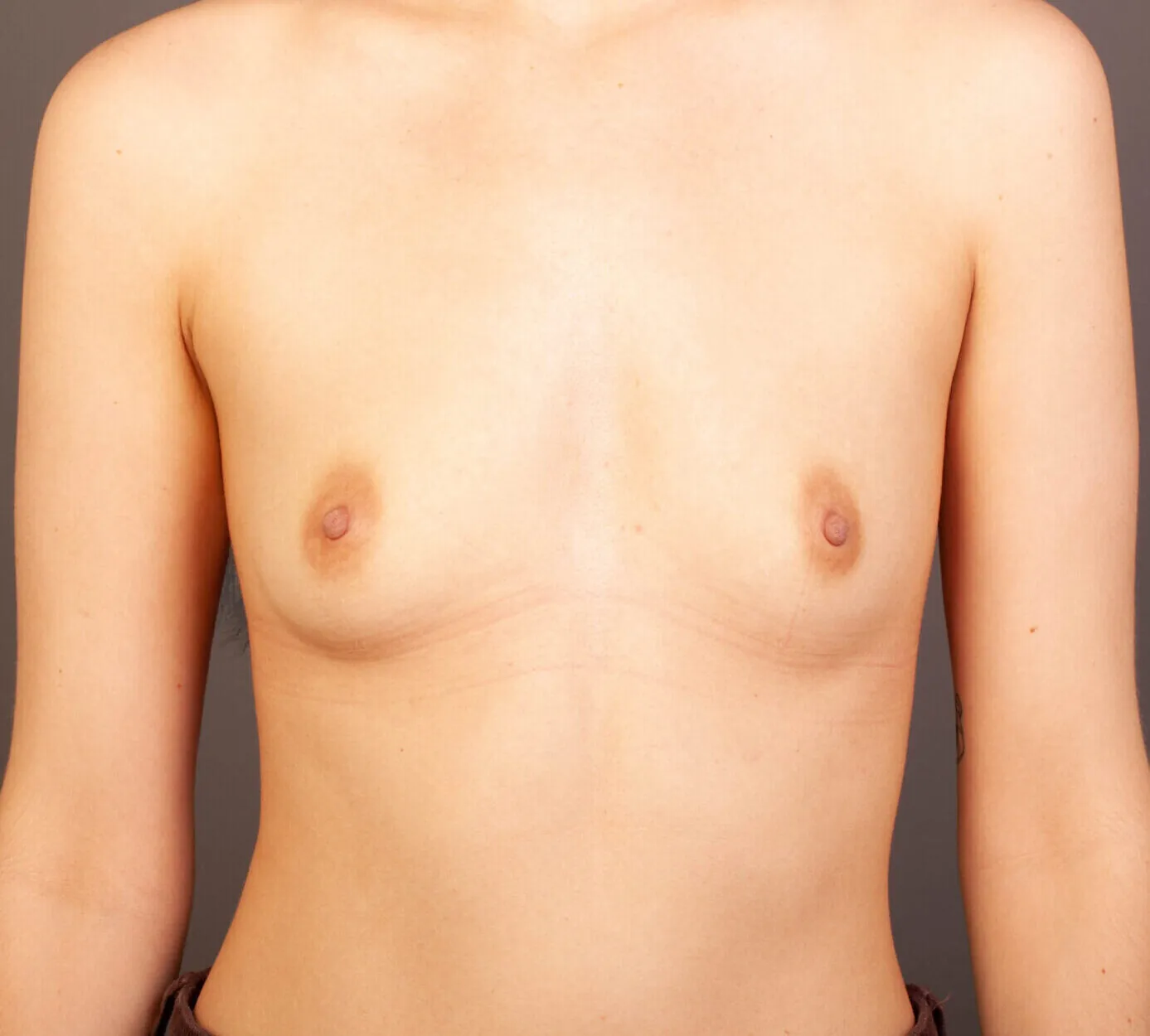
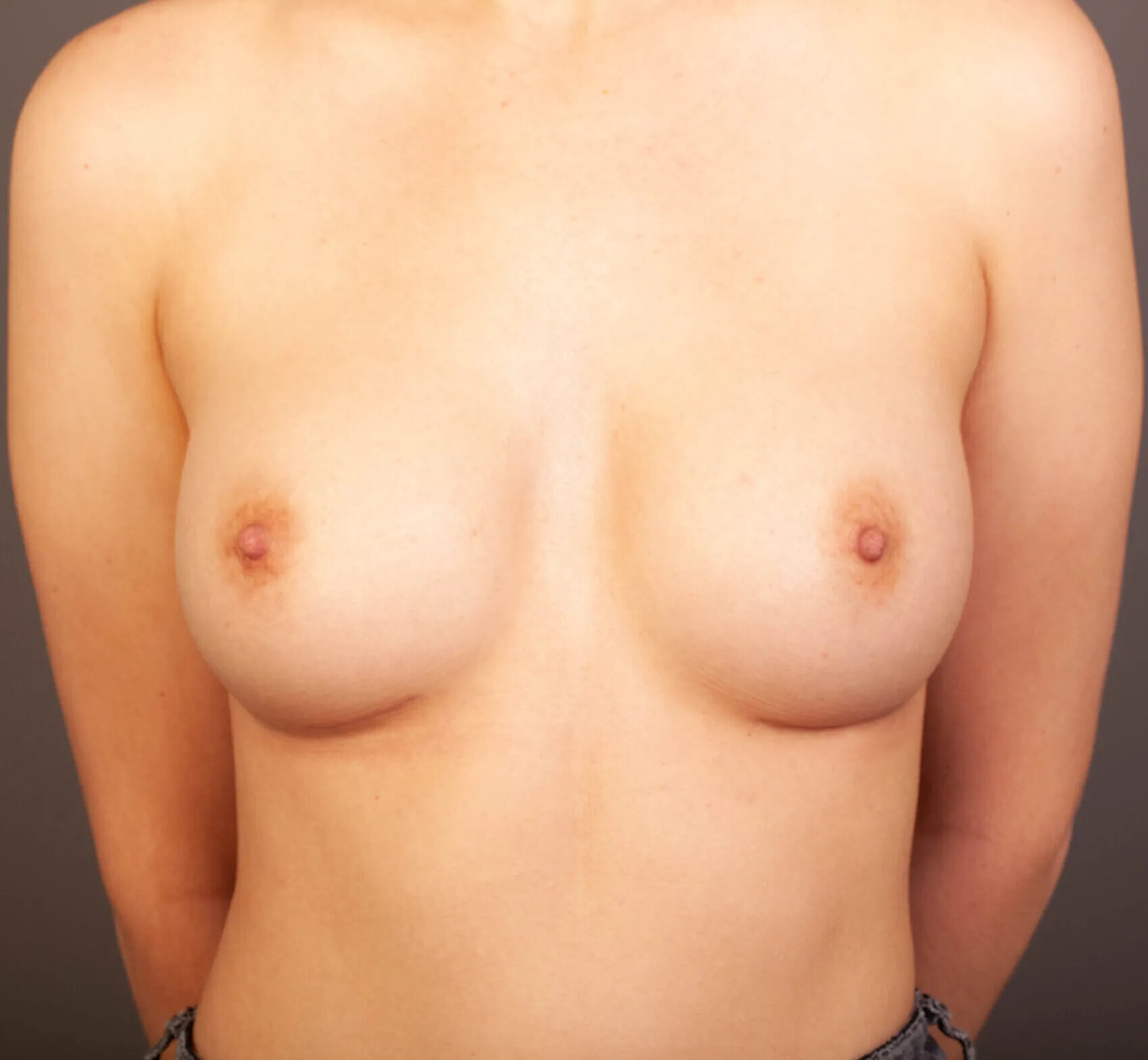
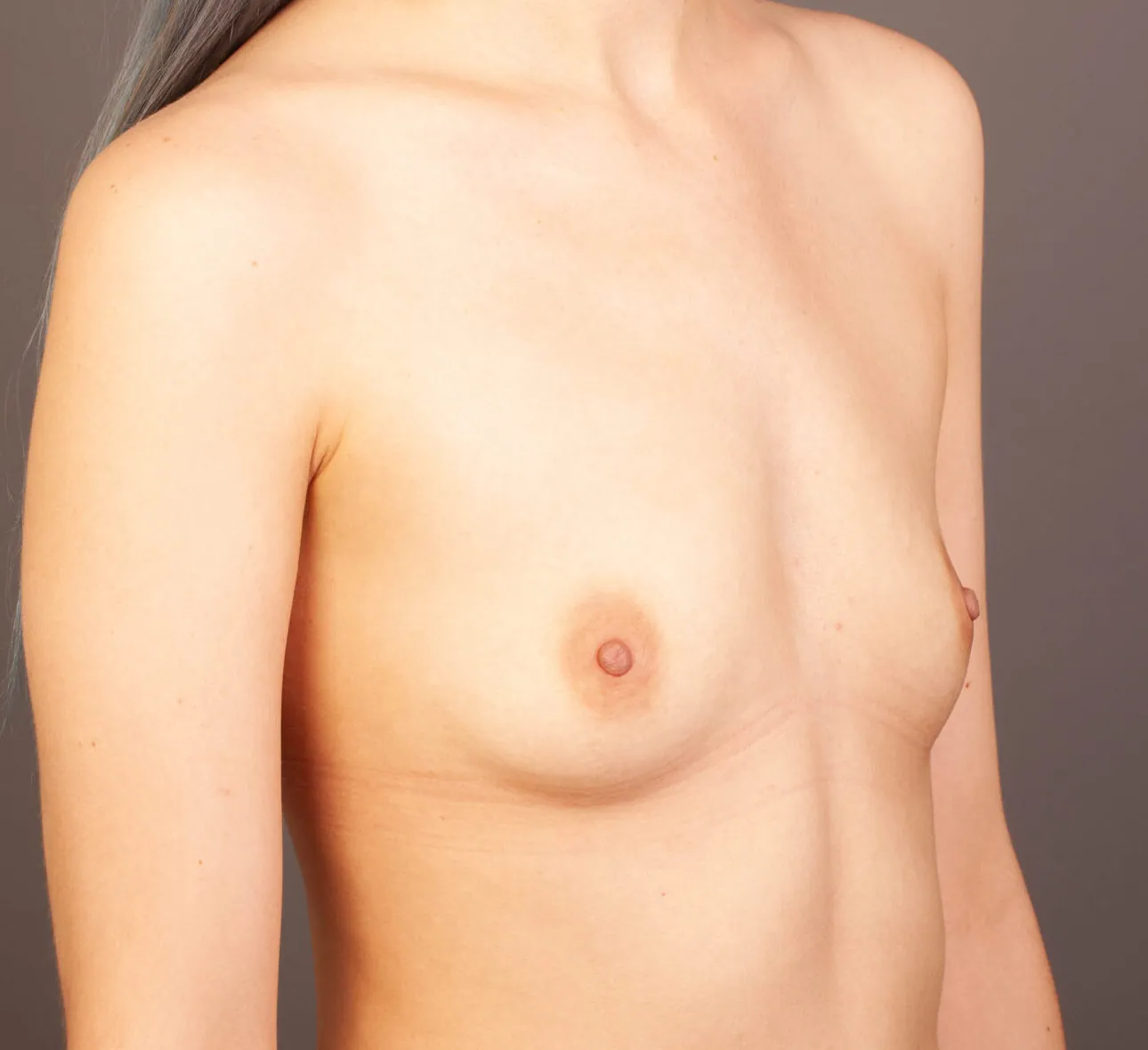
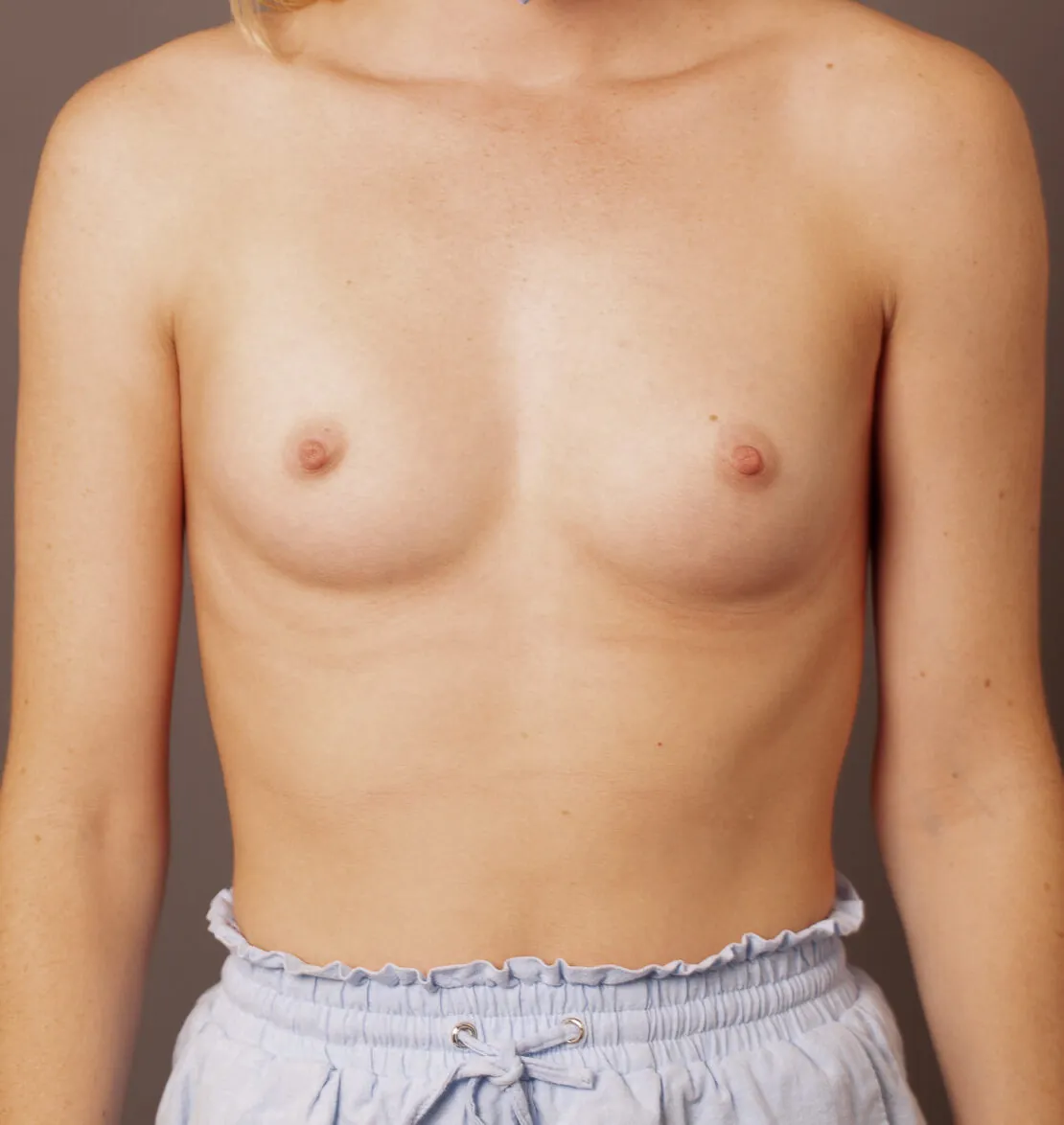
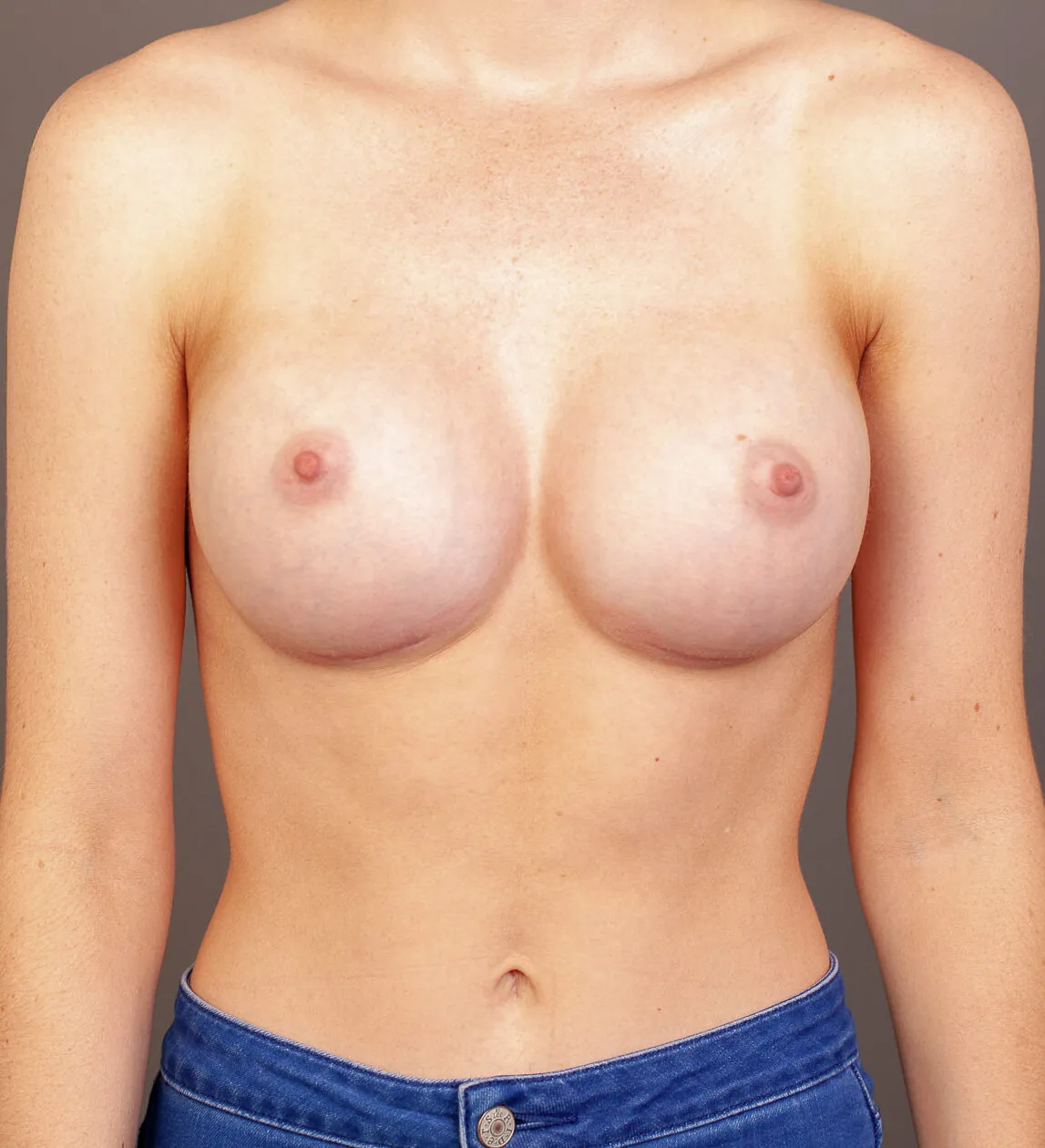
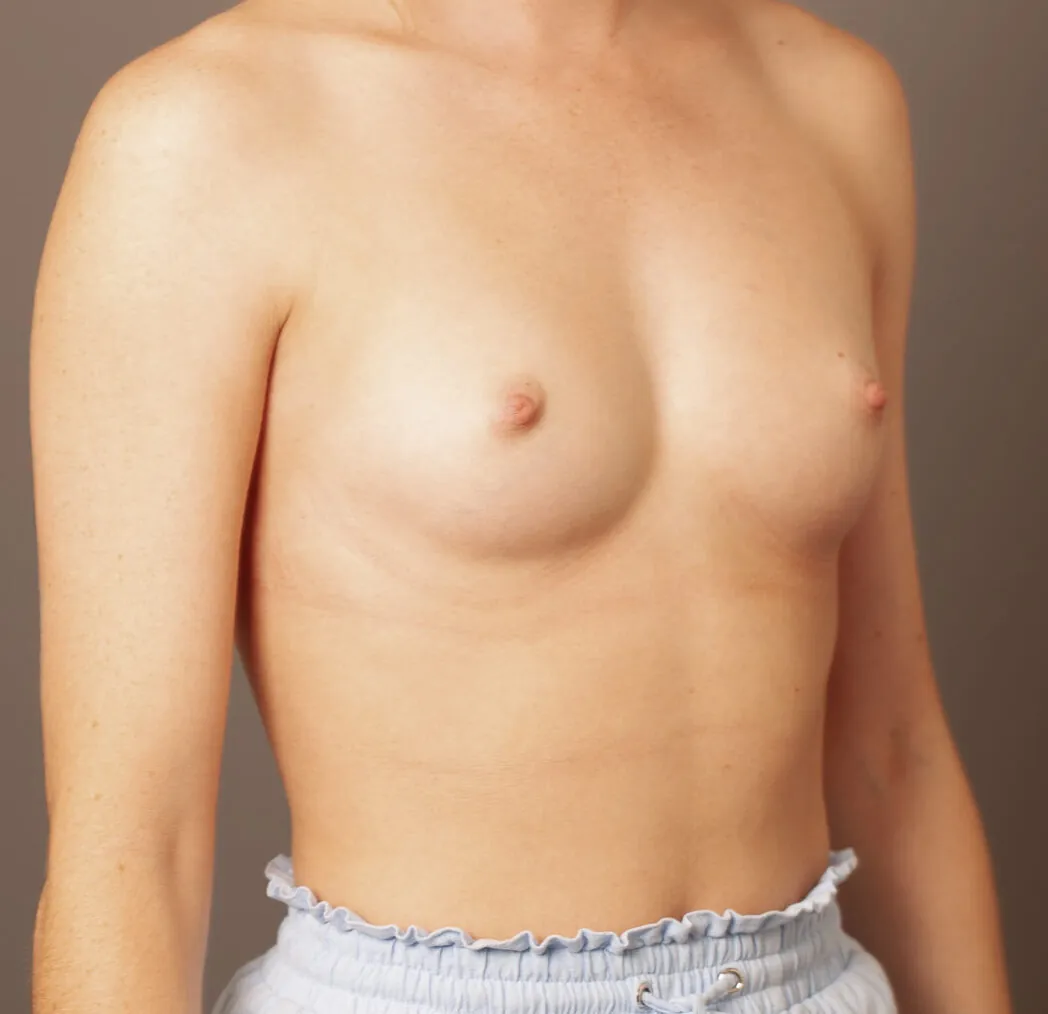
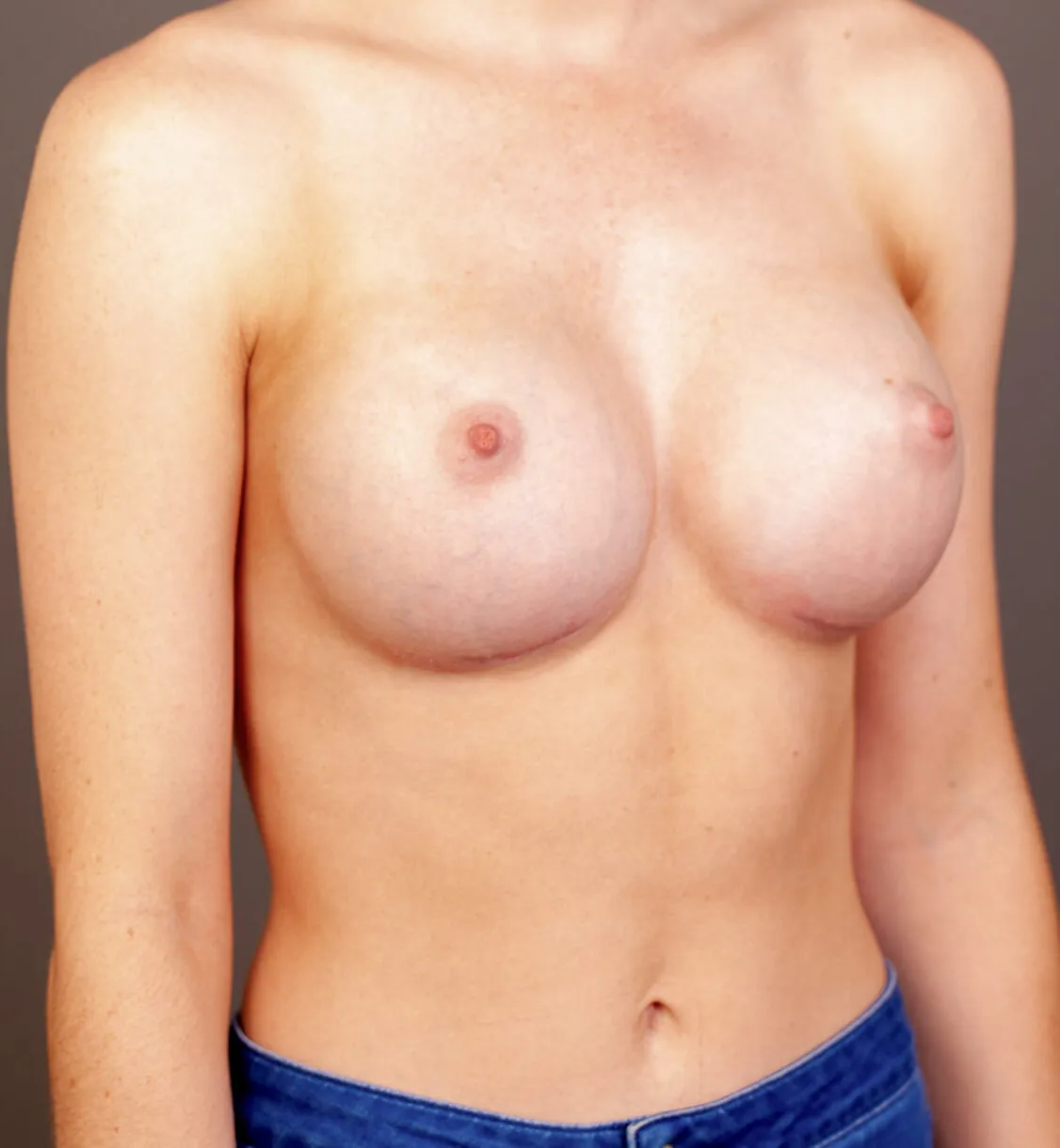
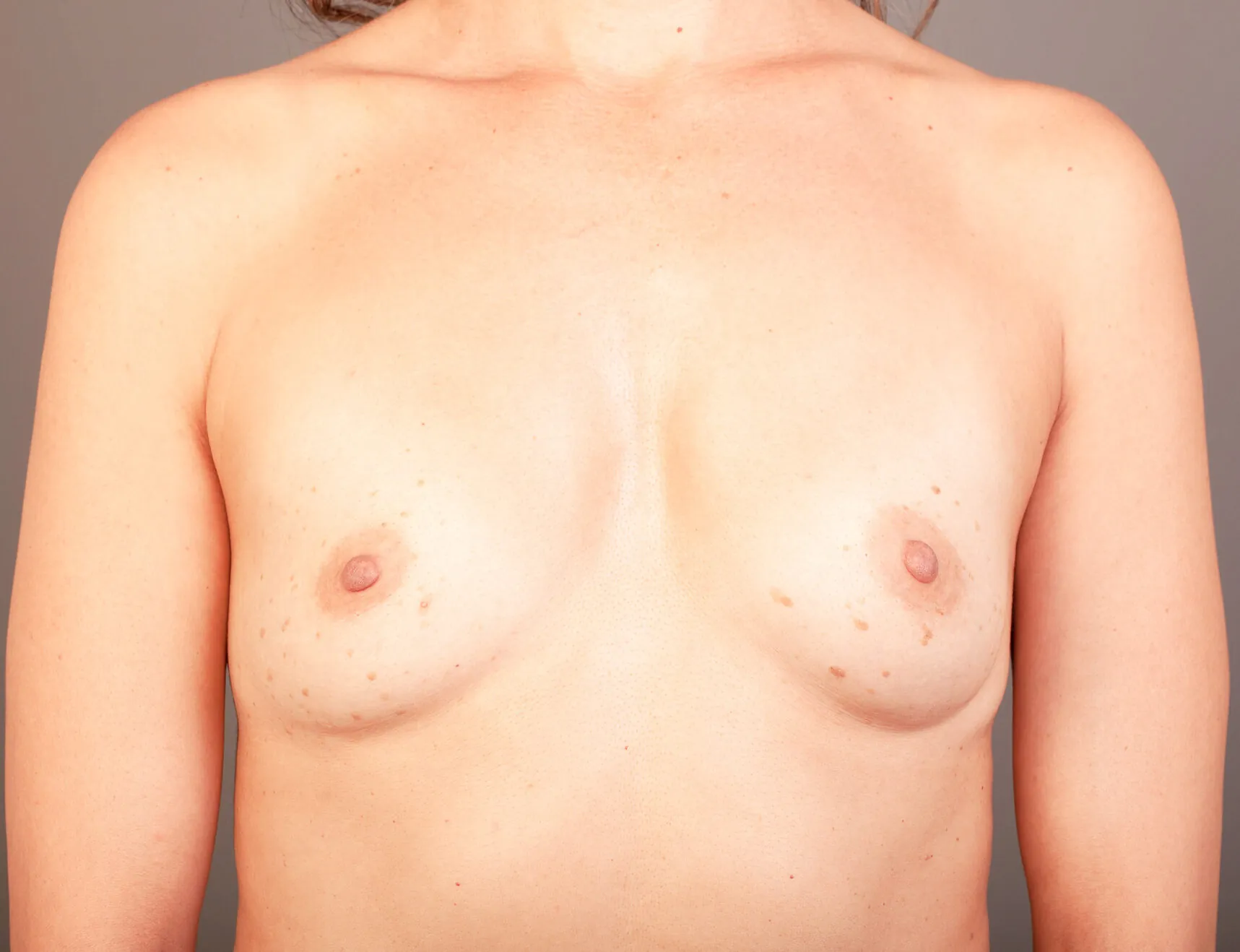
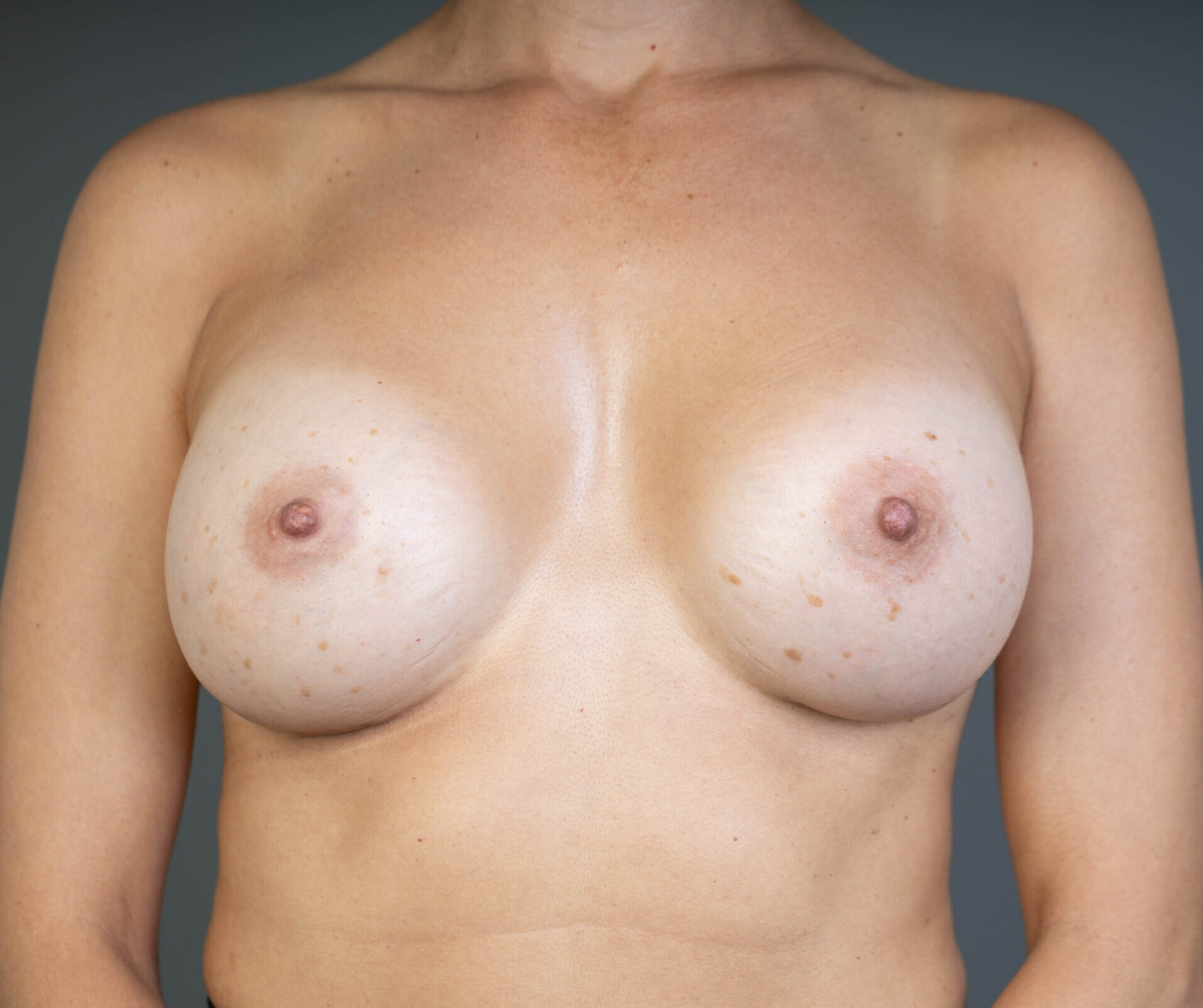
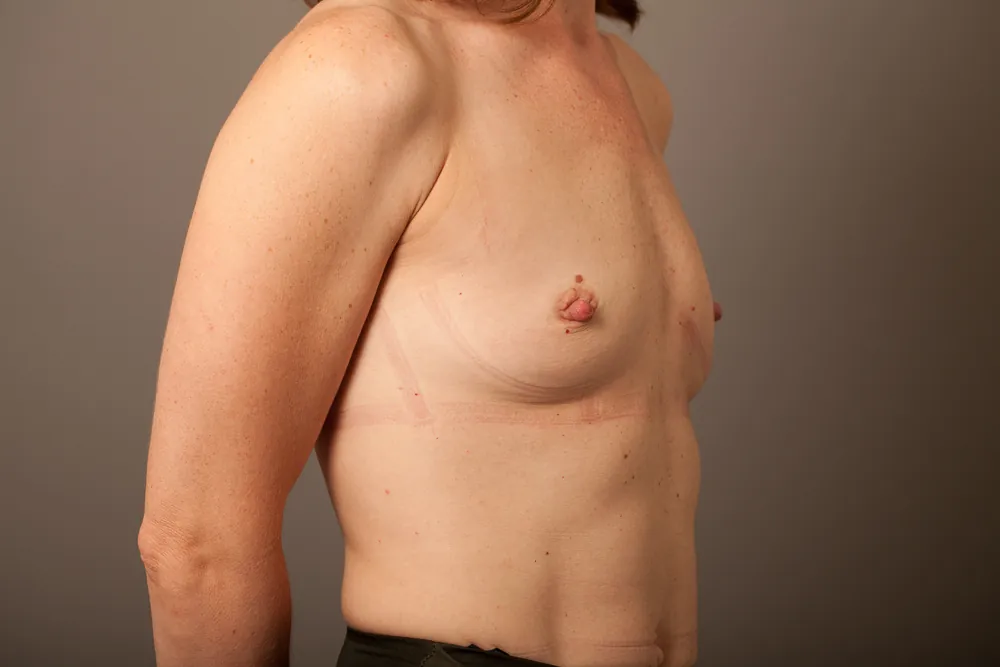
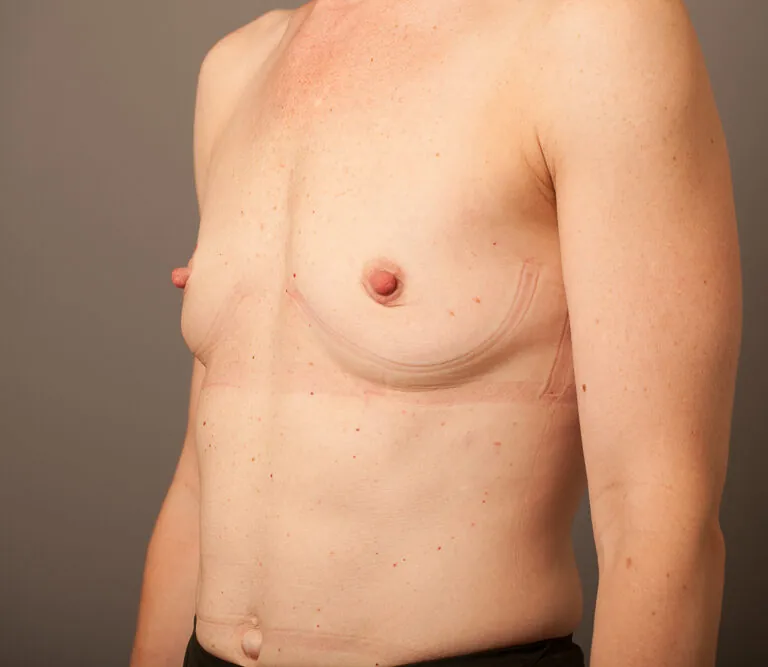
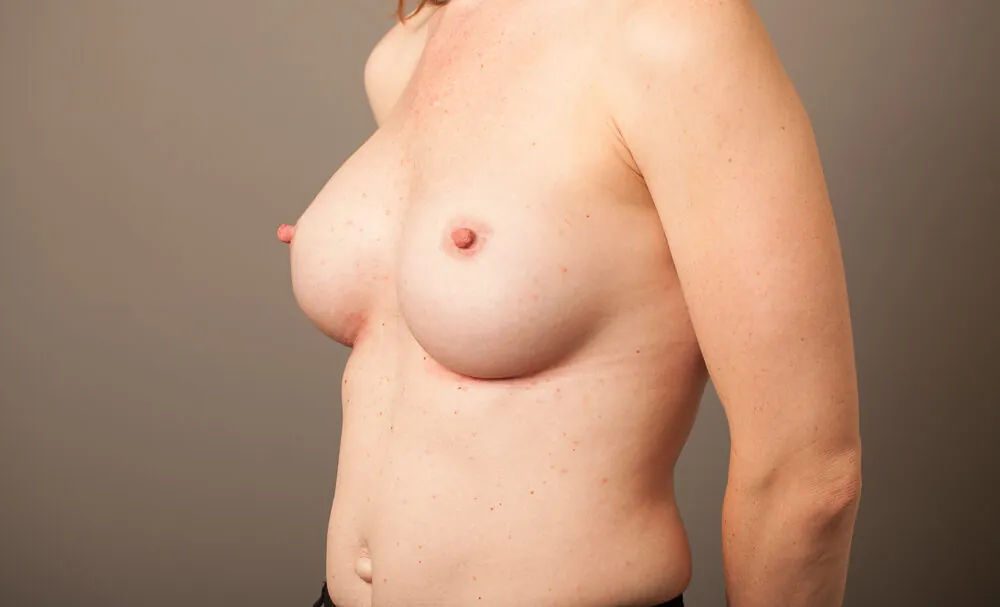
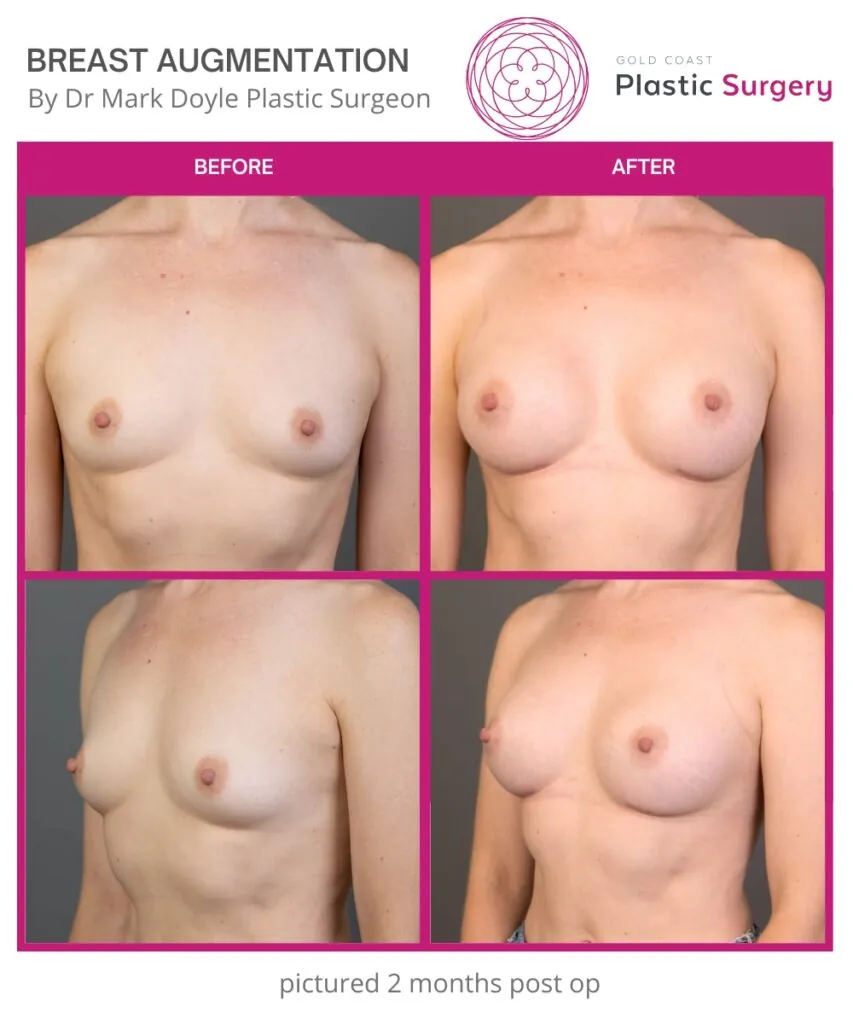
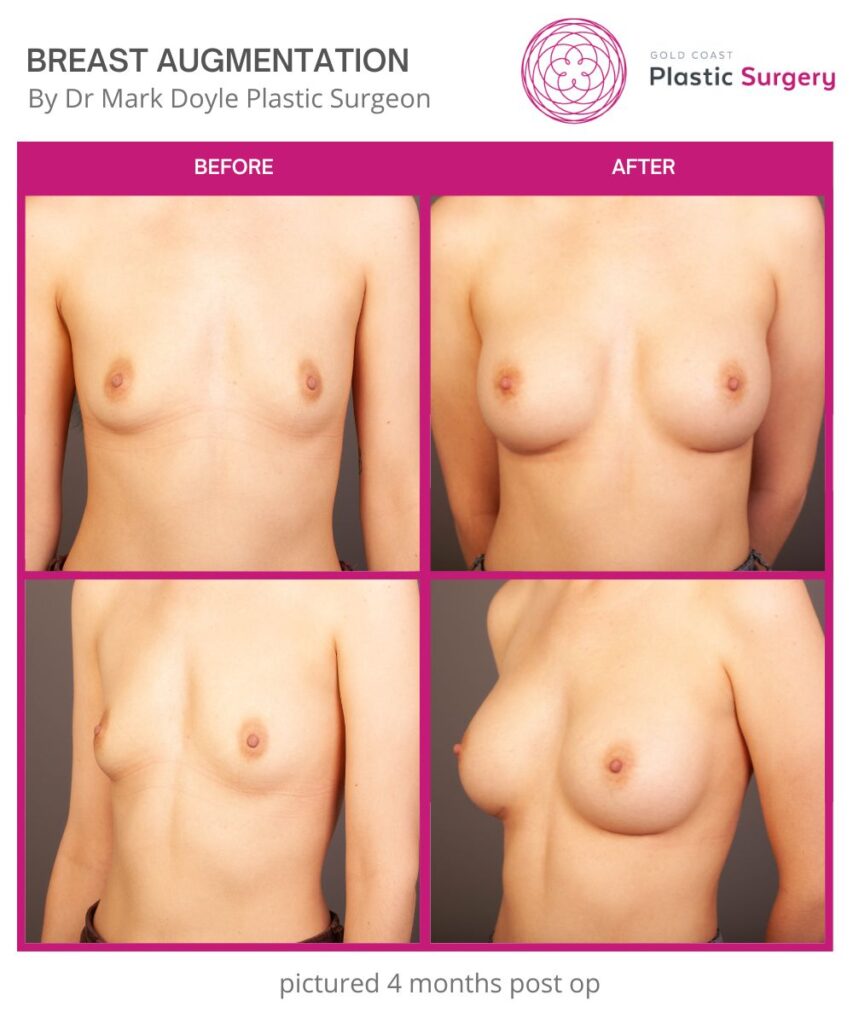
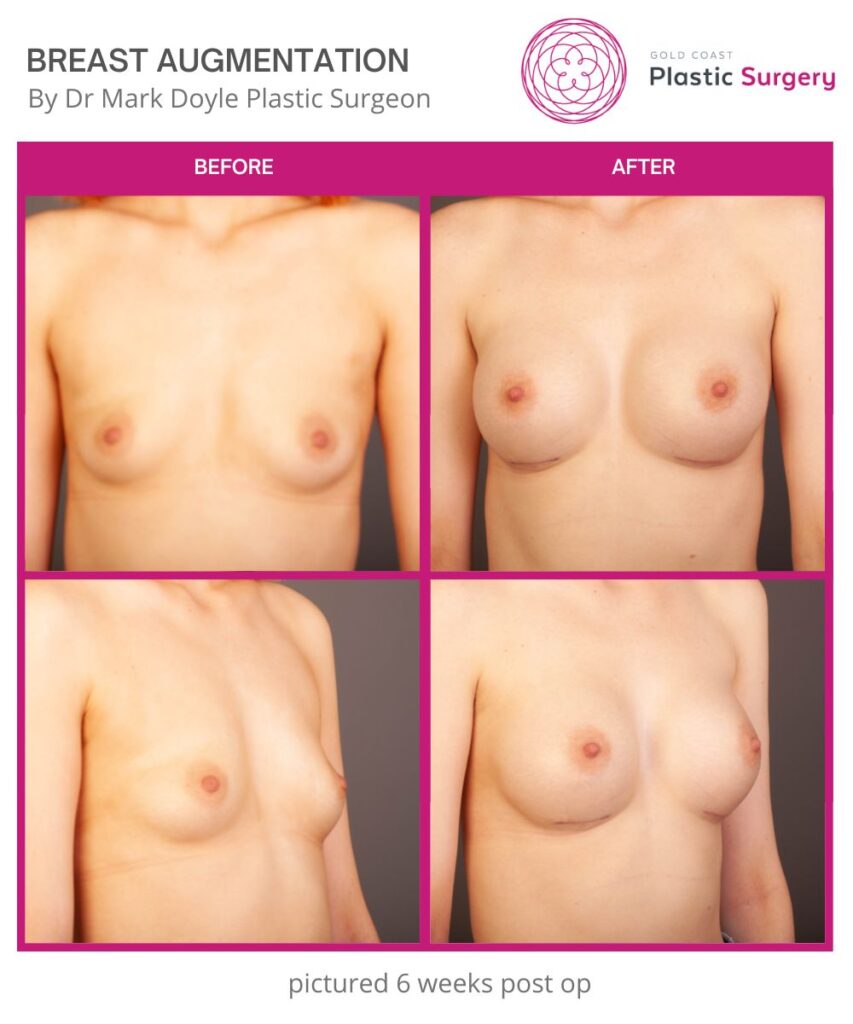
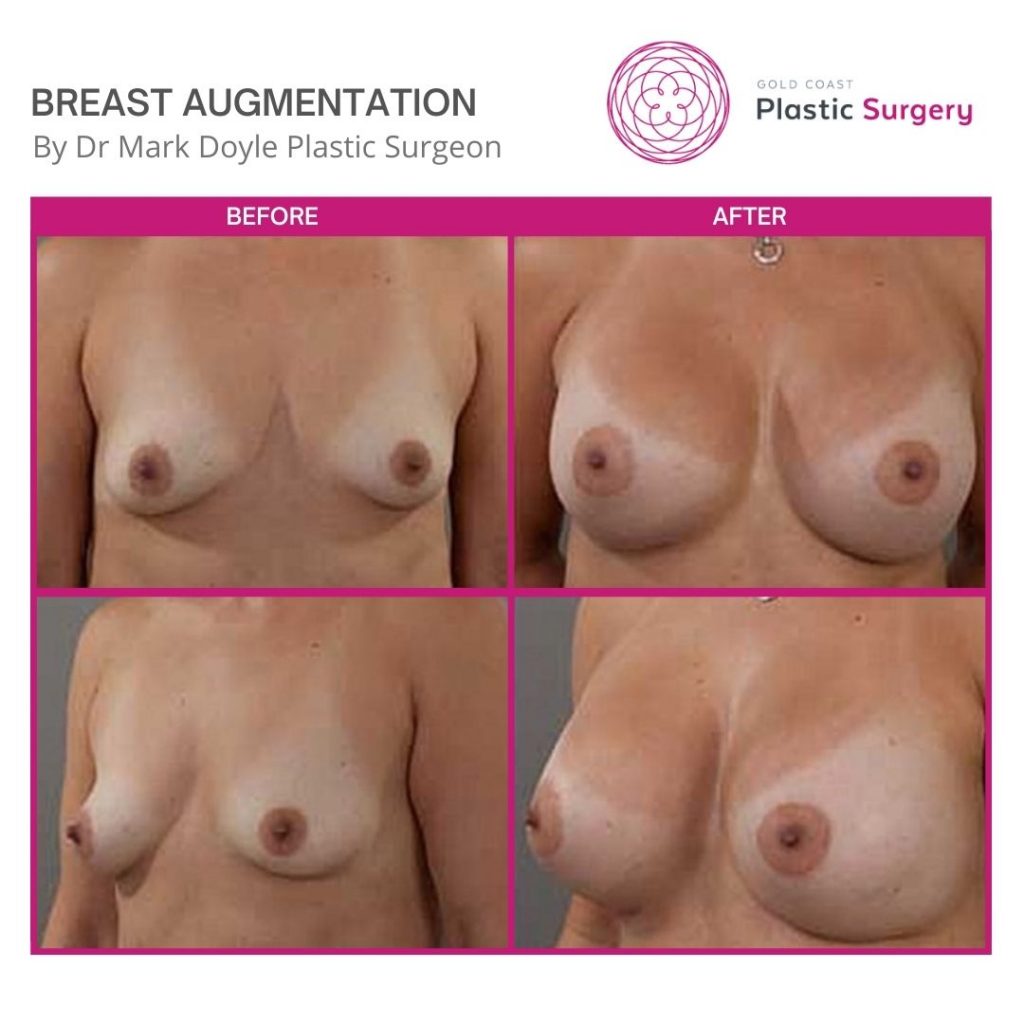
Breast Augmentation Before and After Gold Coast
Disclaimer: All information on the Gold Coast Plastic Surgery website is general in nature and is not intended to be medical advice, nor does it constitute a doctor-patient relationship. Results can vary significantly and depend on individual patient circumstances. Please be aware that the outcomes shown are specific to those patients and may not necessarily reflect the results others may experience. Individual results can vary due to many factors, including genetics, diet, and exercise. All images on this website, unless specified as real patient images, are graphics used for illustrative purposes only. Surgery risks and complications will be covered in detail during a consultation with your surgeon. Book a consult for details regarding your cosmetic surgery procedure.

Breast Augmentation

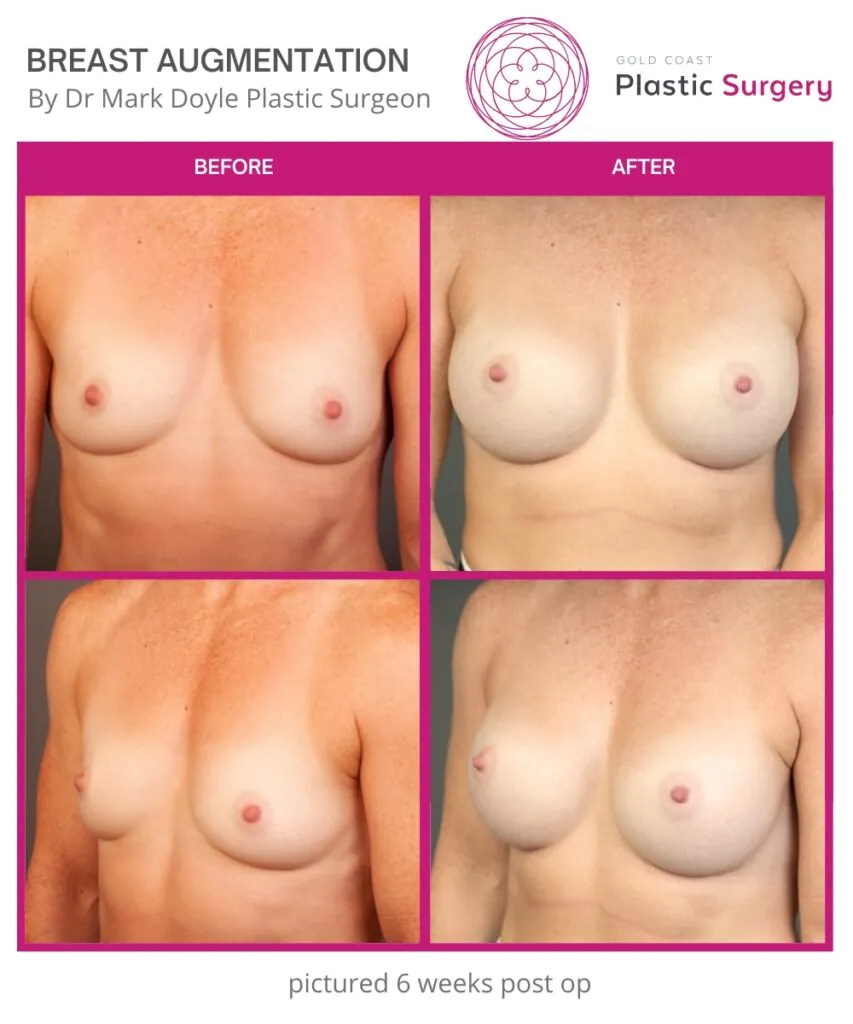
Breast Augmentation

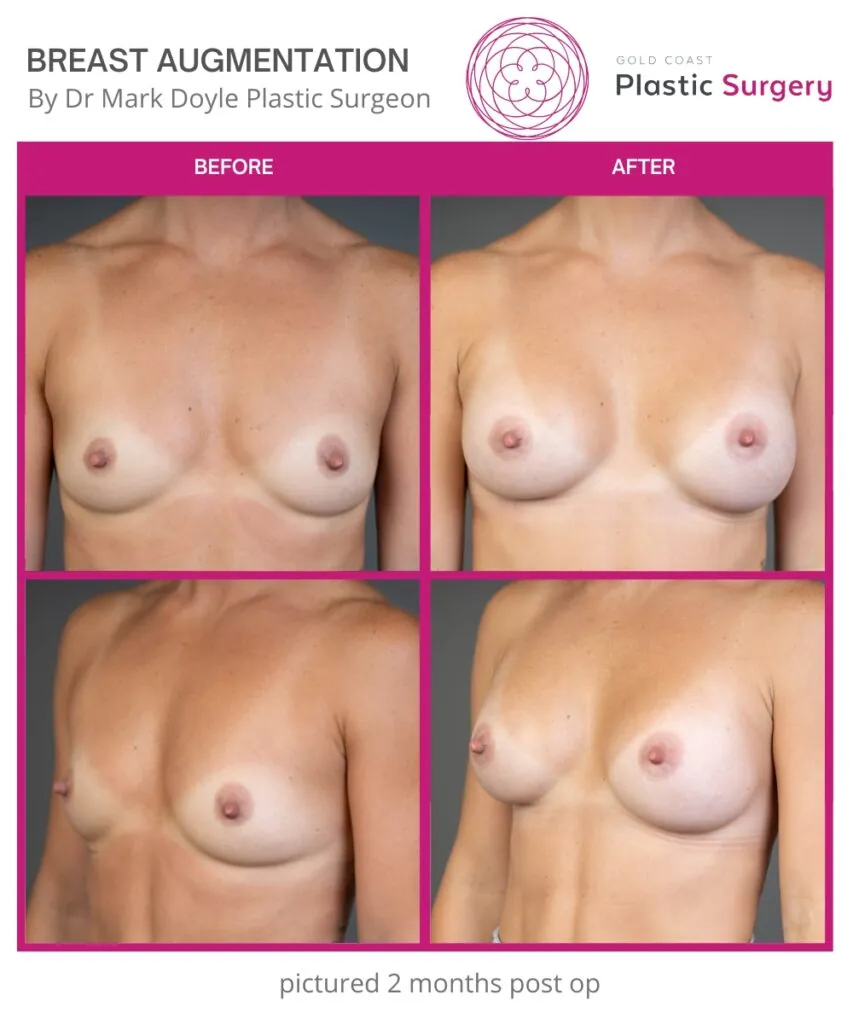
Breast Augmentation

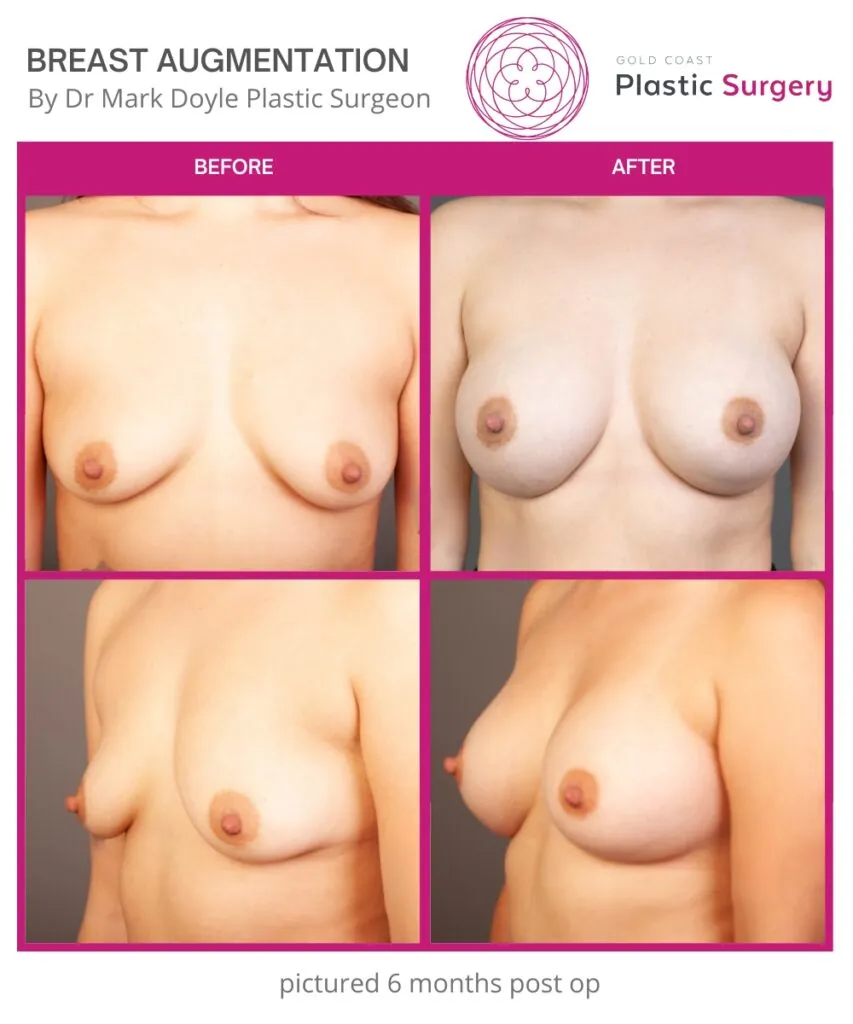
Breast Augmentation

Breast Augmentation

Breast Augmentation
View all Breast Augmentation Before and After
Breast Augmentation Procedure
As mentioned above, during breast augmentation surgery, Dr Doyle creates a space (or pocket) under the breast. He will place the implant behind or in front of the chest muscle, depending on your surgery plan.
Generally, most patients receive dissolvable stitches, Specialist Plastic Surgeon Dr Mark Doyle performs breast augmentation surgery as a day surgery on the Gold Coast.
1. Surgical General Anaesthesia
Medications are administered for your comfort during the surgical procedure. All surgical procedures are performed under general anaesthesia at an accredited hospital. Dr Mark Doyle will recommend the most suitable options for you.
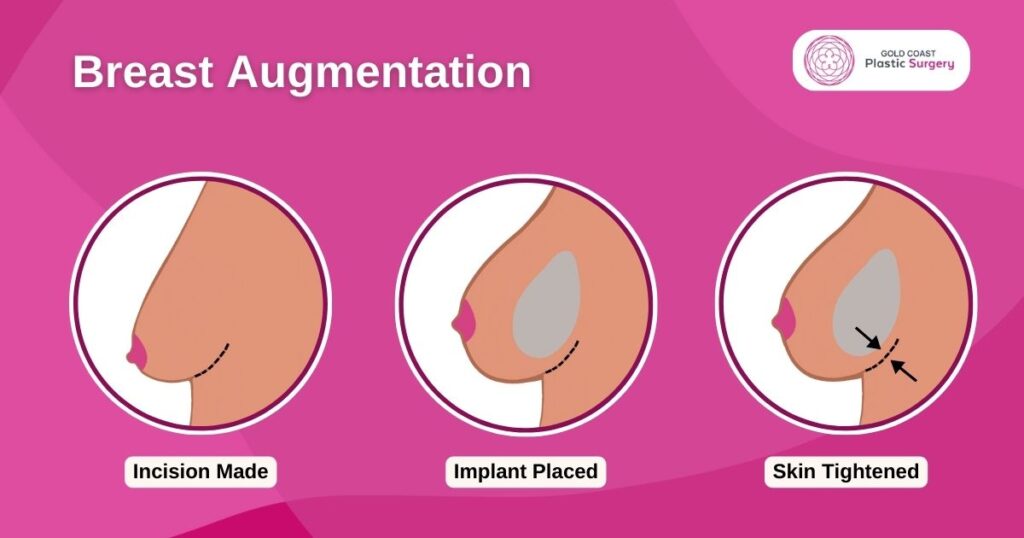
2. Making The Incision
Incisions are made in discreet areas to minimise visible scarring, where possible. Dr Doyle will discuss with you which incision options are appropriate for your preferred surgery outcome. Incisions vary based on the type of breast implant, degree of augmentation preferred and your particular anatomy.
3. Inserting and Placing The Breast Implant
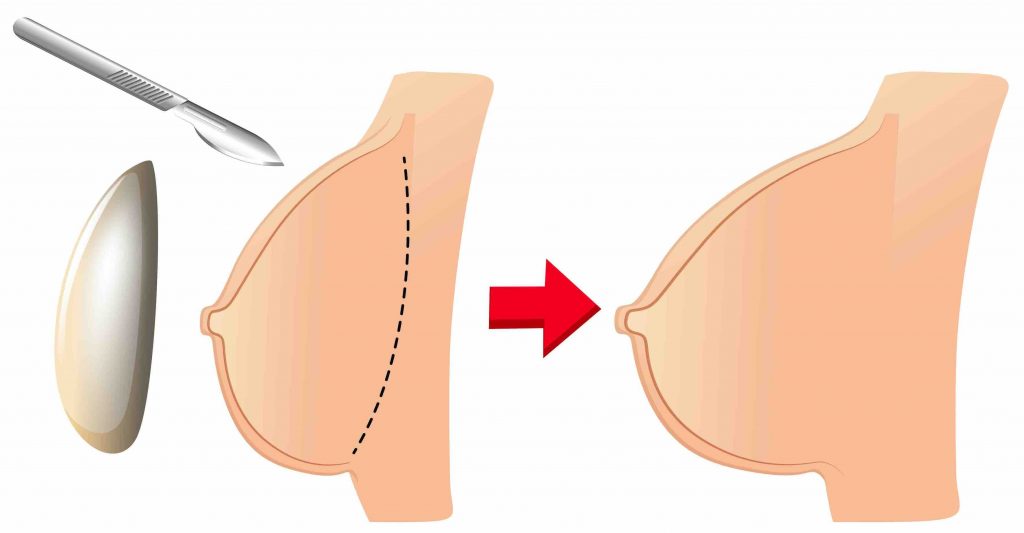
After the incision is made, Dr Doyle will insert the breast implant into a pocket either:
- Under the pectoral muscle (a submuscular placement) or;
- Directly behind the breast tissue, over the pectoral muscle (a submammary/ subglandular placement)
The method for inserting and positioning breast implants depends on the type of implant, degree of augmentation preferred, and your body type and Dr Doyle will finalise it before performing the surgery.
4. Closing The Incisions
Incisions are closed with layered sutures in the breast tissue. Over time the incision lines (scars) will fade. The appearance of the scar depends on many things, including your genetics, exposure of your body to nicotine, sun exposure and infection.
5. Post-Surgery Recovery
Breast augmentation recovery, a crucial phase in this cosmetic procedure, usually lasts up to 12 weeks. We recommend taking a week off work for optimal healing, generally, most pain subsides within the first week. While temporary discomfort and swelling may persist for 1 – 4 weeks. It is crucial to avoid strenuous exercise and heavy lifting during the entire 4-week recovery period to ensure for adequate healing.
Breast Implants Cost
When considering breast augmentation surgery, understanding the cost factors and the potential insurance coverage is important. Here’s a breakdown of the key aspects to consider:
Medicare Rebate for Breast Augmentation Surgery
Medicare rebates for breast augmentation will be available in certain circumstances. However, it’s important to note that breast augmentation is generally considered a cosmetic procedure and may not be covered by Medicare unless it is deemed medically necessary due to congenital deformity, breast reconstruction following mastectomy, or other approved indications. It is advisable to consult with your surgeon and Medicare to determine if you meet the eligibility criteria for a rebate.
Breast Augmentation Cost Considerations
When researching breast augmentation surgery prices, there are several factors to consider. Here’s a breakdown of the key aspects to consider, starting from a base cost of $16,000.
- Surgeon’s experience: Experienced and senior plastic surgeons may charge higher fees.
- Hospital fees: These fees cover the use of the operating theatre, nursing staff, and related services.
- Anesthesia fees: The cost of anesthesia services provided by an anaesthetist.
- Implant type and quality: The cost of breast implants can be influenced by various factors, including the shape, brand, size, and specific features of the implants.
- Post-surgery expenses: It’s important to consider the expenses associated with the post-surgery recovery period, such as medications, follow-up appointments, and supportive garments or bras.
To receive an accurate cost estimate for your breast Augmentation surgery, it is advisable to schedule a consultation with a specialist plastic surgeon. During the consultation, the surgeon will assess your unique case and provide a personalised cost breakdown based on your specific needs and the recommended procedures.
FAQs
How Long Do Breast Implants Last?
The average lifespan of older breast implants is about 20 – 25 years. Newer implants have not been available for this length of time, although it is expected that they will last longer than the original implants. However, this does vary from person to person and depends on which implant type and where the implant is placed. It is important to remember that the quality of the implant is also a factor in its lifespan. Gold Coast Plastic Surgery Plastic surgeon Dr Mark Doyle only uses the Motiva breast implants.
How Do I Choose the Size of My Breast Implants?
Dr Doyle uses Crisalix 3D imaging technology in his breast augmentation consultations. This allows you to trial different virtual breast implant sizes and shapes, to envision how they may fit with your body shape. This 3D before-and-after technology allows you and Dr Doyle a probable preview of the expected cosmetic results from your breast augmentation procedure.
“I use 3D planning tools on breast patients to assess breast volume and asymmetry before surgery and to allow the patients to have more input into the results they prefer with their surgery. 3D simulation of results using different size implants can be important in making an informed decision regarding breast implant size,” says Dr Doyle.
Is It Possible to Combine Multiple Plastic Surgery Procedures?
Yes, breast augmentation surgery can be combined with Breast Lift surgery to address breast ptosis and excess breast tissue. This procedure is known as Breast Lift with Implants Surgery. It is a procedure that Dr Doyle is highly experienced in performing. Also, breast lift before and after photos will give you more understanding of a surgeon’s experience with the procedure.
This procedure also can be combined with Tummy Tuck surgery. It is recommended for women who have finished their families and want to repair their pre-pregnancy bodies from damage, such as, muscle separation.
Gold Coast Plastic Surgeon Dr Doyle may be able to perform Breast Augmentation and Rhinoplasty within the same surgical procedure, as well as other facial surgeries.
Will My Breasts Look Higher After a Breast Augmentation?
While Dr Doyle strives to achieve optimal results for his breast augmentation patients, the outcome is dependent on your goals for the surgery.
“My surgical technique and implant choice both in terms of projection, size and round vs teardrop shapes, will change depending on whether you prefer a more subtle look or glamour look. The positioning of breast implants above or below the pectoral muscles will also affect the final result,” says Dr Mark Doyle.
Can I Get Really Large Implants?
Please note, that Dr Doyle does not use implants larger than one litre in size. You can discuss your size options within a surgery consultation session.
“For those patients considering having larger breast implants to lift the breasts, I would advise them that having larger implants will increase the risk of the implants dropping due to gravity. In these cases a breast lift is generally recommended to give the patients an optimal result. Larger, heavier implants are much more likely to give rise to complications and the need for further surgery,” says Dr Doyle.
Do Breast Implants Drop?
Implants shift and wear over time due to the realistic movement of your body. Larger implants and therefore, heavier implants, are more likely to drop with time. Pregnancy, breastfeeding and weight changes will also influence the position of the implants. This means you may have to replace your implants at least once if you prefer them positioned high. You should always ensure you visit a plastic surgeon who uses TGA-approved breast implant products.
Do I Need to Wear a Bra After Breast Augmentation?
A post-operative bra is recommended and provided for patients to wear for the first six weeks. This surgical garment supports the breasts and promotes healing. It is recommended that patients refrain from driving for at least two weeks after undergoing breast augmentation surgery and avoid partaking in rigorous exercise for at least six weeks.
Can I Breastfeed After Breast Augmentation?
All breast surgery procedures have the potential to affect the nerves and ducts within the breast, which impacts lactation. Breast implants placed below the muscle usually have less effect on milk production than implants placed above the muscle.
It is usually possible to breastfeed after breast augmentation. The type of surgery and in particular, the incisions used for your surgery, can impact your ability to breastfeed.
This is something you must consider before having surgery. If you are planning on having children, you need to weigh up the possibility you won’t be able to breastfeed your child.
Which Type of Breast Implant Is Right for Me?
There are three main types:
- Saline: Filled after insertion with smaller incisions, please note, that Dr Doyle no longer uses these breast implants.
- Silicone: These implants are made from silicone and are preferred by Dr Doyle,
- Gummy bear: Similar to silicone, please note, that Dr Doyle no longer uses these breast implants.
Specialist Plastic Surgeon Dr Mark Doyle will discuss these options and sizes during your appointment, allowing you to try different sizes with a specialised bra for an implant size trial of your potential surgery results.
What Are the Risks of Breast Augmentation?
With modern breast augmentation surgery, the risks have been minimised over the years. However, there is no such thing as risk-free surgery. The important thing is to understand all of the potential risks and take the appropriate steps, in order to minimise them. Any surgical procedure carries some risk of infection, severe bruising, or reaction to anaesthesia.
In the case of breast augmentation surgery, there is also the possibility of complications related to the breast implant, such as rupture, rippling, or capsular contracture. Risks include:
- Capsular contracture (a tightening of the scar tissue that can make the breast feel hard and can distort the shape of the breast implant).
- Changes in nipple and breast sensation (usually temporary).
- Breast pain
- Rare implant leakage or rupture
Am I Too Old To Undergo Breast Augmentation Surgery?
While most breast augmentation patients tend to be in their 20s or 30s, many women choose to have implants inserted in their 40s and 50s. Regardless of your life stage, if you feel that you would like to consider breast implants, schedule a consultation.
Can I Undergo Breast Augmentation Surgery If I Have Excess Breast Skin?
Excess breast skin, also known as ptosis, shouldn’t deter you from undergoing breast augmentation surgery. If the loose skin is severe, you may be recommended to also undergo a breast lift, to achieve an optimal result. This procedure is called a breast lift with implant surgery. If excess skin is not removed, the implants will only cause the breasts to drop even further. Dr Doyle can advise you whether a lift will also be recommended once your breasts and surgery goals have been evaluated.
Is There a Loss of Nipple Sensation if You Get Breast Implants?
The breast implant surgery placement method can influence your risk of sensation loss. Incisions made under the areola pose a higher risk of numbness, whereas incisions under the breastfold typically result in less pronounced numbness. Complete loss of sensation is rare. Following the recovery process precisely, minimise these risks. Dr Doyle will explain his techniques to minimise the risk of complete nipple sensation loss during your surgery consultation.
Book a consultation
Dr Mark Doyle offers breast augmentation surgery to all patients in Brisbane, Sunshine Coast and Gold Coast. To find out if breast surgery is right for you, book a consultation with Gold Coast Plastic Surgery today. Patients from all around Queensland and Byron Bay, Northern NSW are welcome to visit us at Gold Coast Plastic Surgery on the Gold Coast.
About Dr Mark Doyle FRACS (Plas) – Queensland Plastic Surgeon
Servicing patients in Gold Coast, Brisbane, Sunshine Coast, Cairns and New South Wales NSW – Northern Rivers, Byron Bay, Ballina, Lismore and more.
Dr Mark Doyle is a fully qualified Specialist Plastic Surgeon with over 30 years of experience performing breast, body, face and nose surgery. He has completed all required training and only carries out approved surgical practices. There are NO undertrained doctors or cosmetic doctors acting as surgeons at Gold Coast Plastic Surgery.